Learn More About Dry Eye
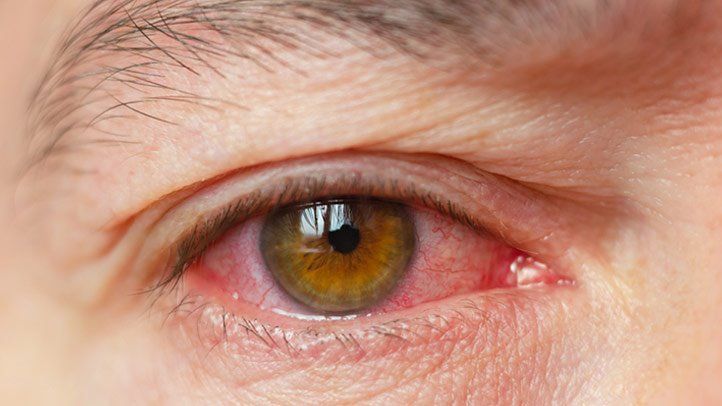
Dry eye disease (DED) is a multifactorial disorder of the ocular surface characterised by loss of tear film homeostasis, resulting in symptoms of discomfort, visual disturbance, and potential damage to the ocular surface. According to the latest Tear Film & Ocular Surface Society Dry Eye Workshop (TFOS DEWS III), DED arises from a combination of tear film instability, hyperosmolarity, ocular surface inflammation, and neurosensory abnormalities. The condition affects millions worldwide and has significant implications for quality of life, productivity, and ocular health. Risk factors include aging, female sex, autoimmune disorders (e.g., Sjögren’s syndrome), contact lens wear, environmental stress, prolonged screen use and medications.
Classification
DED is broadly classified into two major subtypes, which often overlap:
- Aqueous-Deficient Dry Eye (ADDE):
This form results from inadequate tear secretion by the lacrimal glands. It may occur due to systemic autoimmune diseases such as Sjögren’s disease or non-Sjögren’s causes including lacrimal gland dysfunction, aging, or certain medications. - Evaporative Dry Eye (EDE):
This type is more common than ADDE and occurs when tear evaporation exceeds normal levels, primarily due to meibomian gland dysfunction (MGD), which leads to an unstable lipid layer. Environmental factors such as low humidity, air conditioning, and digital device use also exacerbate evaporative loss.
Many patients present with mixed-type dry eye, involving features of both aqueous deficiency and increased evaporation.
Treatment Overview
Management of DED aims to restore tear film stability, reduce inflammation, and relieve symptoms. Treatment is typically staged based on disease severity:
- Lifestyle and Environmental Modifications:
Reducing screen time, optimising ambient humidity, using protective eyewear, and ensuring adequate hydration are essential first steps. - Artificial Tears and Lubricants:
Over-the-counter lubricating drops, gels, and ointments help replenish tear volume and improve comfort. Preservative-free formulations are preferred for frequent use. - Management of Meibomian Gland Dysfunction:
Warm compresses, lid hygiene, and in-office procedures such as thermal pulsation or intense pulsed light (IPL) therapy can improve meibomian gland function. Twice daily warm compress and lid massage has been proven effective in managing chronic MGD and is the current standard of care for evaporative dry eye. - Anti-inflammatory Therapy:
Topical corticosteroids (short-term), cyclosporine A, and tacrolimus ointments target underlying ocular surface inflammation. These are often introduced in moderate to severe cases. It is important to note that topical steroids are not for long-term use due to their complications such as increased eye pressure and risk of glaucoma and cataract. - Tear Conservation and Stimulation:
Punctal plugs may be inserted to reduce tear drainage, and secretagogues (e.g., diquafosol, pilocarpine) can stimulate tear production. - Advanced and Adjunctive Therapies:
Autologous serum eye drops, scleral lenses, and systemic immunomodulatory therapy may be indicated in severe cases, particularly those with autoimmune aetiologies.
Dry eye disease is a complex, multifactorial condition requiring individualised assessment and management. Early recognition and a stepwise, evidence-based treatment approach are essential to prevent chronic ocular surface damage and improve patients’ quality of life.
Our clinic specialises dry eye diagnosis and management using the latest evidence-based approach such as IPL and gland expression. Phone us to make an appointment.